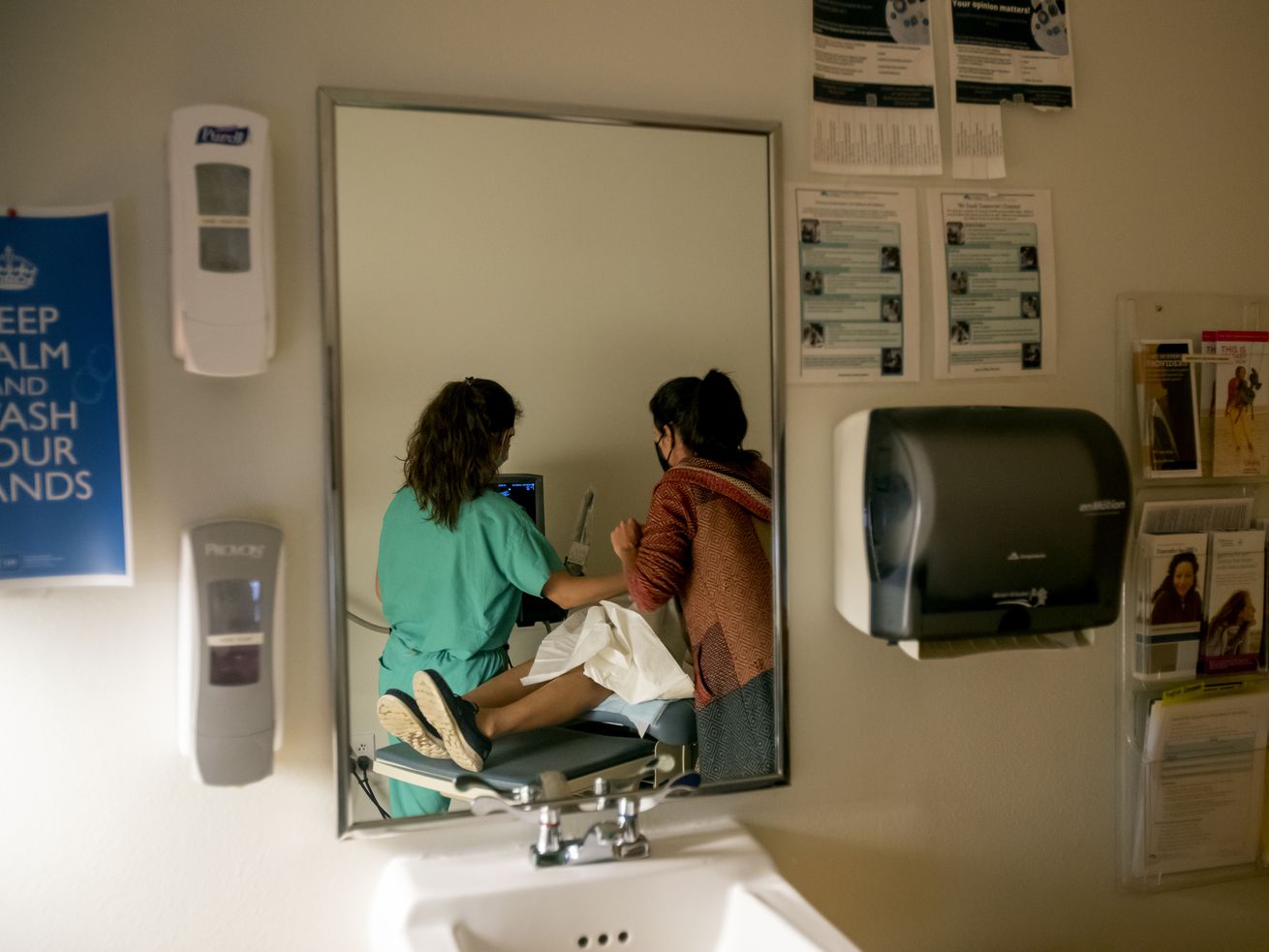
Why medical emergency exceptions for abortions aren’t enough.
Even before the Supreme Court overturned Roe v. Wade on June 24, stripping Americans of their right to an abortion, the United States had an abysmally high maternal mortality rate, ranking last in a survey of 10 similarly wealthy countries. For doctors in states implementing restrictive abortion bans, the ruling is a crisis of care: In many cases, the only way to treat life-threatening conditions such as ectopic pregnancies is with medical or surgical termination. The fear among many physicians is that the ruling in Dobbs v. Jackson Women’s Health Organization will make mortality rates creep even higher.
States that are enacting the most stringent abortion bans — like Missouri, where a “trigger law” went into effect the day of the ruling — do make exceptions for medical emergencies. But huge questions remain: How might someone in a medical emergency get a lifesaving abortion in a state with no, or few, providers? And who gets to decide what counts as a “lifesaving” emergency?
Nobody seems to know for sure. But one thing is clear: The ruling raises far more questions than it answers. And while the answers are deliberated, patients around the country stand to suffer unnecessary, debilitating pain or death.
“We’re venturing into unknown territory,” said Lori Freedman, a sociologist and associate professor of obstetrics and gynecology at the University of California San Francisco.
There are a few big categories of unknowns here: how doctors will act if they fear prosecution for providing care, how hospital lawyers will interpret state laws, and who will provide abortions in cases when they are legally allowed to save the life of the pregnant person.
Maternal health care in America is at an inflection point. And with every unknown there is danger.
Fear of prosecution could alter medical decision-making
A pregnancy can be dangerous even in the best of circumstances. “Carrying a pregnancy is more dangerous than not carrying a pregnancy. Birth is riskier than an abortion,” said Jody Steinauer, a physician and director of the Bixby Center for Global Reproductive Health at UC San Francisco. Pregnancy causes a panoply of physiological changes to a person’s body, and problems can arise throughout the process.
The American College of Obstetricians and Gynecologists recommends early abortions for patients with some heart conditions, while patients with diabetes whose fetuses will develop severe anomalies can spend time focusing on controlling their diabetes before trying to get pregnant again. Some complications are apparent far before they begin to affect the vital signs of a pregnant person, Steinauer said. Patients with poorly controlled diabetes are at a higher risk of having fetal anomalies, for example, and patients with mental health issues or cardiac disease can be in serious danger if they carry a pregnancy to term.
The Dobbs ruling will make responding to those problems more difficult. One major source of uncertainty lies in how physicians will respond to the threat of prosecution for performing abortions, even in cases where their patient’s life is in danger. That fear of criminalization could lead doctors to put off care for longer than they would otherwise.
For doctors, a big component of that fear is that determining what’s “lifesaving” isn’t perfectly cut and dried.
“At what point do we say that danger has been triggered?” asked Carmel Shachar, executive director of the Petrie-Flom Center for Health Policy Law, Biotechnology, and Bioethics at Harvard Law School. “That’s really unclear, and it’s very hard for providers because they want to provide timely medical care.”
What constitutes danger, and when, varies patient by patient. If a patient has a missed miscarriage, for example, where the fetus has stopped developing but the pregnant person hasn’t experienced any symptoms such as bleeding, they can develop sepsis, which is when their body starts damaging itself as an extreme response to an infection. The treatment for a missed miscarriage is removing the fetal tissue — in other words, an abortion — and is best done as early as possible.
But without the protections of Roe, doctors may be forced to wait to take action until their patient’s condition deteriorates. “Do you need to wait for the patient to become septic before you can act?” Shachar asked.
As Anna North wrote for Vox in 2019, some abortion opponents argue that complications like missed miscarriages and ectopic pregnancies should be left to “resolve on their own.” Doctors in states with abortion bans may feel they have no choice but to stand back and wait.
“What’s really important and sad is that you really can’t keep the patient’s best interest in mind,” said Freedman. “Her suffering is not accounted for at all. Even if they can keep her from having long-term harm, she’s still going to have worse care. She’s still going to be stalled and scared for longer.”
Do doctors get to make the call, or do lawyers?
Even before the Dobbs ruling, deciding whether to perform an abortion, especially in states with restrictive abortion laws, would often become a discussion that went beyond the physician and patient to include a hospital’s legal team and sometimes even a department chair or board of administrators. But those discussions happened with the knowledge that, fundamentally, Roe v. Wade guaranteed that patients had a right to an abortion and doctors faced minimal risk of prosecution for performing them in response to a medical emergency. Now hospitals will be left on their own to interpret the laws of their states, which could lead to even more confusion.
Physicians and hospital lawyers have a difficult job ahead in figuring out how to comply with the law, partly because the language used in the abortion debate and the laws that come out of it have little basis in medical science, said Louise Perkins King, a physician at Brigham and Women’s Hospital in Boston and director of reproductive bioethics at Harvard Medical School’s Center for Bioethics.
When lawmakers talk about heartbeats and fetal viability, for example, they do so in a way that is totally different from how physicians use those words. Texas law, for example, mentions the “dead, unborn child,” but “that’s a word that means nothing to me as an obstetrician, because I deal in the words of ‘embryo,’ ‘fetus,’ and perhaps ‘neonate,’” King said.
That disconnect between medical science and policy means that without clarification from state attorneys general, hospital lawyers will have to make case-by-case decisions on whether their physicians can provide abortions — and they’ll probably err on the side of extreme caution, delaying or denying patients the care they need. Many of these debates may simply come down to a matter of personality: If a hospital has a director who strongly supports abortion rights, for example, they could be more permissive. This is, of course, ludicrous — a patient’s right to care should not depend on the whims of hospital management.
Even if there is legal clarity, there may not be ethical clarity. “It may be that in your state, what is legal is in direct conflict with providing the best health outcomes for your patients,” said Shachar. “I think it’s going to be really complicated and really hard for providers to work through what happens when they know what the standard of care is, but they’re legally not able to provide it.”
Where will abortions even occur?
Before the Dobbs ruling, doctors at hospitals with restrictive abortion policies had the option to send their patients to other facilities, like abortion clinics or different hospitals, that could perform emergency abortions instead. That’s what would happen at Catholic hospitals, said Freedman, who has extensively studied abortion policies in Catholic hospital systems. “But that was a very different context,” she said. Before June 24, those doctors were protected by Roe; even if they ran the risk of losing their jobs, they were never at risk of being criminally prosecuted for doing their jobs.
That has changed.
Some doctors have already indicated they’re willing to provide abortions to their patients, even if it means they risk being prosecuted, said King. But that could present even more problems: If a doctor is charged with a crime, their license will be suspended, which means their patients — even those who might not need abortions — won’t get the care they need.
Steinauer is also concerned about what will happen if and when freestanding abortion clinics are forced to close. “Many communities have these great independent abortion clinics that are providing wonderful care for our patients, and the local hospital does not necessarily need to be involved, especially in earlier abortion care,” Steinauer said.
In the past, those clinics would often handle abortion care in the first trimester of pregnancy, including cases where patients had to get abortions for conditions like cardiac disease, while hospitals and academic institutions would usually take patients in their second or third trimesters. Without those clinics providing support, hospitals might become overloaded with patients they aren’t used to seeing. Care for those patients could then be delayed or even denied, based on the decisions a hospital’s legal team comes to.
The Food and Drug Administration has approved drugs that can be used to induce an abortion, and it may be possible to continue receiving them via telehealth across state lines even if states pass sweeping bans on surgical abortions (an ongoing federal lawsuit may provide more clarity on this soon). US Attorney General Merrick Garland has promised to protect Americans’ access to these medications, which means it could remain a good option for many patients and may help reduce the burden of those clinics closing, but it’s still not a perfect solution.
Abortion pills can cause complications in rare circumstances, and King worries patients may choose to delay care or be afraid to tell their doctors about what medicines they took. That’s going to disproportionately affect people of color, who already face medical bias. “My biggest fear is that somebody’s going to take those meds at home because they don’t have any other choice and then have a hemorrhage and be too scared to come in,” said King.
It’s likely many of these questions will only be answered once they make their way back to the Supreme Court, which Shachar says is an inevitability. But that will take months, if not years.
It’s hard to predict what kind of damage will be done in the meantime. “It’s hard to imagine Americans will tolerate women dying,” said Freedman. “I feel like doctors will get loud if it’s truly causing deaths. But there’s so much we don’t know. We never thought we would see this day.”
0 Comments